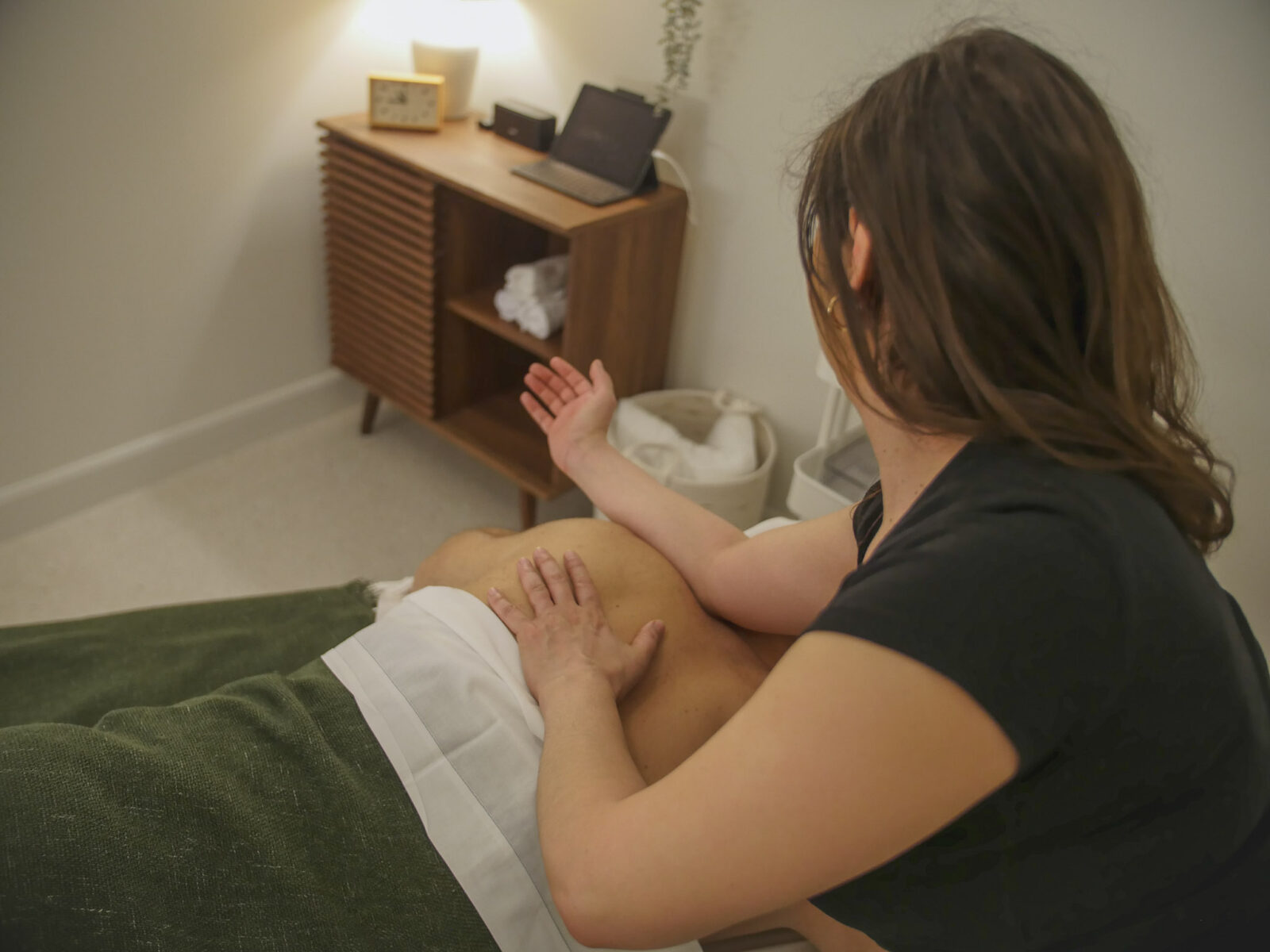
You press on a spot in your shoulder and suddenly feel pain shoot into your neck. Or you have a persistent ache in your upper back that no amount of stretching seems to touch. These are classic signs of trigger points — and they’re more common than most people realize.
Trigger point therapy is one of the most effective tools for resolving this kind of pain. Yet it’s also one of the most misunderstood. This article covers what trigger points actually are, why they form, and how a trained RMT treats them.
What Are Trigger Points?
A trigger point is a hyperirritable spot within a taut band of muscle tissue. When compressed — or even when left alone in active cases — it produces local pain and often refers pain to a predictable distant site. Notably, referred pain patterns are what distinguish trigger points from general muscle soreness.
Dr. Janet Travell and Dr. David Simons first mapped trigger points systematically. Their work through the latter half of the 20th century documented consistent referral patterns for hundreds of muscles. For example, a trigger point in the upper trapezius reliably refers pain up the side of the neck and into the temple. Meanwhile, a trigger point in the infraspinatus refers into the front of the shoulder and down the arm — often mimicking a rotator cuff injury or even cervical nerve compression.
Because of this referred pain behaviour, people often seek treatment for the symptom site — the neck, the headache, the shoulder — rather than the source. As a result, trigger point therapy works by identifying and treating the actual origin of the pain.
What Causes Trigger Points?
Trigger points form when a region of muscle tissue stays in sustained contraction — what researchers call a contracture. A failure of the normal calcium-pump mechanism that allows muscle fibres to relax drives this process. Several factors can initiate it:
• Acute overload — a sudden force or strain that overwhelms the muscle’s capacity
• Chronic overuse — repetitive movement patterns that accumulate microtrauma over time
• Sustained postures — prolonged sitting, screen work, or any fixed position that loads specific muscles continuously
• Direct trauma — a blow, fall, or compression injury that initiates a contracture in the affected tissue
• Emotional stress — which raises baseline muscle tone and predisposes tissue to trigger point development
• Deconditioning — muscles that are weak relative to their demands develop trigger points more readily
In many cases, trigger points develop quietly over months or years before becoming symptomatic. By the time a client notices a problem, multiple active and latent trigger points are often contributing to the pattern.
Active vs. Latent Trigger Points: What’s the Difference?
Not all trigger points behave the same way. Understanding the distinction helps explain why some pain patterns are constant and others only appear under specific conditions.
Active Trigger Point | Latent Trigger Point | |
Pain at rest? | Yes — spontaneous, often constant | No — only painful when compressed or stressed |
Referral pattern? | Yes — produces referred pain spontaneously or on compression | Possible on compression, but not at rest |
Movement restriction? | Often significant — muscle guarding and reduced range | Mild to moderate — contributes to stiffness without acute pain |
Latent trigger points matter clinically because they lower the threshold for active trigger point development. Consequently, a region with multiple latent trigger points is primed to become acutely painful under relatively minor stress. Many people are surprised to find their pain flares up out of proportion to what caused it — latent trigger points are often the reason.
Common Tension Points in the Back — and What’s Behind Them
The back is the most common region where clients report trigger point pain. However, the specific location tells you a lot about which muscles are involved — and where the actual source is.
Upper Back and Between the Shoulder Blades
Desk workers and people who spend long hours on screens most commonly report pain in this area. The rhomboids and middle trapezius are frequently involved. However, the source is often the scalenes and anterior neck muscles, which refer pain posteriorly.
In addition, sustained forward head posture loads the levator scapulae, producing a deep ache at the top of the shoulder blade that many people mistake for neck pain.
Lower Back
Lower back tension points often originate in the quadratus lumborum — a deep muscle running between the last rib and the top of the pelvis. QL trigger points refer into the SI joint region, the buttock, and sometimes the hip. As a result, these patterns are commonly misdiagnosed as sciatica or disc-related pain.
The iliopsoas, which runs through the front of the body, also refers into the lower back. Because its trigger points are not directly accessible from the posterior surface, clinicians frequently overlook them.
Mid-Back
The thoracic erectors and multifidus often drive mid-thoracic pain. In addition, trigger points in the serratus anterior — located on the side of the ribcage — can refer into the mid-back. Pain here is frequently missed because its location doesn’t match the source. Furthermore, intercostal trigger points can produce a band-like tightness that wraps around the trunk.
How Trigger Point Release Works
Trigger point release involves applying precise, sustained pressure directly to the hyperirritable spot within the taut band. Held for several seconds to a minute or more, this input disrupts the contracture cycle. It also allows blood flow to return to the ischemic tissue and signals the nervous system to reduce local motor tone.
RMTs use several methods in practice:
• Ischemic compression — sustained direct pressure that temporarily occludes local blood flow, followed by reactive hyperemia when pressure releases
• Stripping — a slow, firm stroke along the length of the taut band from the trigger point toward the muscle’s origin or insertion
• Contract-relax techniques — the muscle contracts gently against resistance, then releases, before pressure reapplies; this often allows deeper access with less discomfort
• Integrated neuromuscular inhibition — combines compression with positional release and muscle energy techniques for complex or resistant trigger points
Your RMT selects the approach based on which muscle is involved, how sensitive the tissue is, and how long the trigger point has been present. Chronic trigger points generally require a gentler, longer approach than acute ones.
What to Expect During Trigger Point Therapy
Trigger point work has a distinctive sensation. When the therapist locates an active trigger point and applies pressure, you may feel the referred pain pattern reproduce — discomfort in your neck from shoulder work, or arm heaviness from a posterior shoulder trigger point. Reproducing this referral pattern confirms the location and shows the treatment is working.
The pressure can be intense, but it should not be sharp or unbearable. The goal is to work at the threshold of comfortable intensity — what some practitioners describe as a “good hurt.” Bracing against the pressure prevents release, so breathing through it and letting the tissue respond produces better outcomes.
After treatment, the area may feel tender for 24 to 48 hours — similar to soreness after a hard workout. Most clients notice a meaningful reduction in referred pain and improved range of motion within 24 hours of a session.
Trigger point therapy is often integrated with myofascial release in the same session, since fascial restrictions and trigger points frequently coexist. While myofascial release addresses the broader connective tissue environment, trigger point work targets the specific contracture sites within it.
Who Performs Trigger Point Therapy at Myocare?
All trigger point treatment at Myocare comes from Registered Massage Therapists — regulated health professionals governed by the College of Massage Therapists of Ontario (CMTO). Several of our RMTs specialize in this work, including Adriana Petrik (18+ years, myofascial release and trigger point specialist), Kenny Karst, and Tyler Ruebottom. Our RMTs approach trigger point therapy as part of a broader clinical assessment — not just pressure on sore spots.
We also offer massage therapy for TMJ jaw pain, which often involves trigger point work in the masseter, temporalis, and pterygoid muscles — a specialized application of these techniques.
Frequently Asked Questions
What does trigger point therapy feel like?
When the therapist applies pressure to an active trigger point, you’ll typically feel the referred pain pattern reproduce — a sensation extending to the area where you’ve been experiencing symptoms. Finding the source is actually reassuring, not alarming. Productive discomfort rather than sharp pain is what you should expect. Most clients report significant relief within 24 hours.
How is trigger point therapy different from myofascial release?
Trigger point therapy targets specific contracture sites within a taut muscle band using direct, sustained pressure. In contrast, myofascial release addresses broader fascial restrictions using slow stretch techniques across larger regions. Both treat soft tissue pain, but they work at different levels of the tissue. Together, they are often used in the same session for better results.
Can trigger point therapy help with tension headaches?
Yes — many tension headaches originate from trigger points in the upper trapezius, sternocleidomastoid, suboccipitals, and temporalis. All of these muscles have well-documented referral patterns into the head. Treating these sources directly is often more effective than treating the head itself.
Clients who experience frequent tension headaches often see a significant reduction in frequency and intensity with regular trigger point work.
How many sessions will I need?
Acute trigger points — those that developed recently from a specific incident — often resolve in one to three sessions. In contrast, chronic trigger points that have been present for months or years typically require longer treatment, with gradual improvement across five to eight sessions. Your RMT will reassess after each session and adjust the plan based on how the tissue responds.
Is trigger point therapy covered by insurance in Ontario?
Yes — trigger point therapy by a Registered Massage Therapist is covered under extended health benefits as RMT treatment. Myocare offers direct billing to most major insurers.
Check your plan’s annual RMT benefit limit to understand how many sessions your coverage includes.
What’s the difference between trigger point therapy and acupuncture?
Both approaches can address trigger points, but through different mechanisms and regulatory frameworks. Manual pressure on muscle tissue is what defines RMT-based trigger point therapy. Dry needling — which targets trigger points with thin needles — is a related technique some physiotherapists and acupuncturists use. At Myocare, our acupuncture practitioners use Traditional Chinese Medicine acupuncture, which overlaps with trigger point locations in some cases but follows a different clinical framework.
Book Trigger Point Therapy in Toronto
Myocare RMT & Wellness is at 1096 Bathurst Street in the Annex, open Monday through Sunday. If you’re dealing with persistent muscle pain, recurring tension headaches, or a pain pattern that doesn’t match a clear injury, trigger point therapy may be the right next step. Browse our Practitioners page to find the right RMT, review rates and services, and book online. Call us at (416) 995-6601 with any questions.